Genital herpes is a common sexually transmitted infection caused by the herpes simplex virus (HSV) that leads to recurring sores, blisters, or skin irritation around the genitals and anus.
Many people mistake early symptoms for harmless irritation or genital skin rashes, which is why proper medical assessment and treatment for penile skin rashes matters before symptoms worsen or recur. If you’ve ever had unexplained genital discomfort that comes and goes, this is one condition you shouldn’t ignore.
What Is Genital Herpes?

Genital herpes is a lifelong viral infection most commonly caused by HSV-2, although HSV-1, the virus behind oral cold sores, can also infect the genital area through oral sex. Once the virus enters the body, it stays dormant in the nervous system and can reactivate from time to time.
In Malaysia, genital herpes is often underdiagnosed, not because it’s rare, but because symptoms can be mild, intermittent, or completely absent. Furthermore, the social stigma of getting diagnosed with sexually transmitted diseases (STD) in men is a taboo to plenty. Many only find out after passing it unknowingly to a partner or until the deed is done.
How Does One Get Genital Herpes?

Genital herpes spreads through direct skin-to-skin contact, not through fluids like semen or blood. That distinction matters because it explains why so many people get infected even when they believe they’ve been “careful”.
Sexual contact and skin-to-skin transmission
The virus enters the body through tiny breaks in the skin or mucous membranes around the genitals, anus, mouth, or eyes. Vaginal and anal sex are common routes, but penetration isn’t required for the virus to transmit. Prolonged skin contact with an infected area especially during intimate touching is all that’s needed for disease transmission.
Condoms reduce risk, but they don’t fully eliminate it. Areas not covered by protection can still come into contact with viral particles. This is why people sometimes contract genital herpes despite consistent condom use and no visible signs on their partner. At He Medical Clinic, we highly recommend circumcision for both adults and children as one of the most effective ways to prevent genital herpes.
Can you get genital herpes from oral sex?
Yes, and this is one of the most underestimated transmission routes. Oral cold sores are caused by HSV-1. When oral sex occurs, the virus can transfer from the mouth to the genital area, leading to genital herpes. This can happen even if the cold sore is small, healing, or barely noticeable.
Many people assume that cold sores are “common” because they’re harmless. In reality, HSV-1 has become an increasingly common cause of genital herpes, particularly among people who have never had traditional genital symptoms before.
Can genital herpes spread without visible sores?
This is where genital herpes becomes genuinely tricky. The virus can be active on the skin without causing blisters, pain, or irritation. This process, known as asymptomatic viral shedding, allows transmission to occur when everything looks and feels normal.
Shedding is most frequent during the first year after infection, but can continue long after. Because there’s no visual cue, partners often have no idea exposure has occurred until symptoms appear weeks or months later for people in monogamous relationships.
What Does Genital Herpes Look Like in Real Life?

Genital herpes rarely announces itself in an obvious or dramatic way. In many cases, it creeps in quietly, which is why people overlook the early signs or mistake them for something minor.
Early signs most people ignore
The earliest symptoms often don’t look like an infection at all. People describe a faint tingling, mild itching, sensitivity, or a warm, irritated feeling on the skin. Sometimes there’s slight redness without any visible sores.
Because these sensations are subtle, they’re commonly brushed off as shaving irritation, friction from tight clothing, excessive sweating, or even stress-related skin sensitivity. Heat rashes are often blamed due to our hot, humid weather conditions, especially when symptoms fade after a day or two.
What a herpes outbreak typically feels like
As the outbreak develops, clusters of small blisters may appear. These blisters are usually filled with clear fluid and sit on reddened, tender skin. They’re fragile and can rupture easily.
Once the blisters break, they leave behind shallow open sores that can feel raw and painful. The discomfort brings constant pain with sharp stings or burning sensation, especially during urination, walking, or prolonged sitting.
Over time, the sores scab over and heal on their own. This healing process can take anywhere from one to three weeks, which is why many people delay seeing a doctor under the assumption that the issue has resolved itself.
Genital Herpes in Men
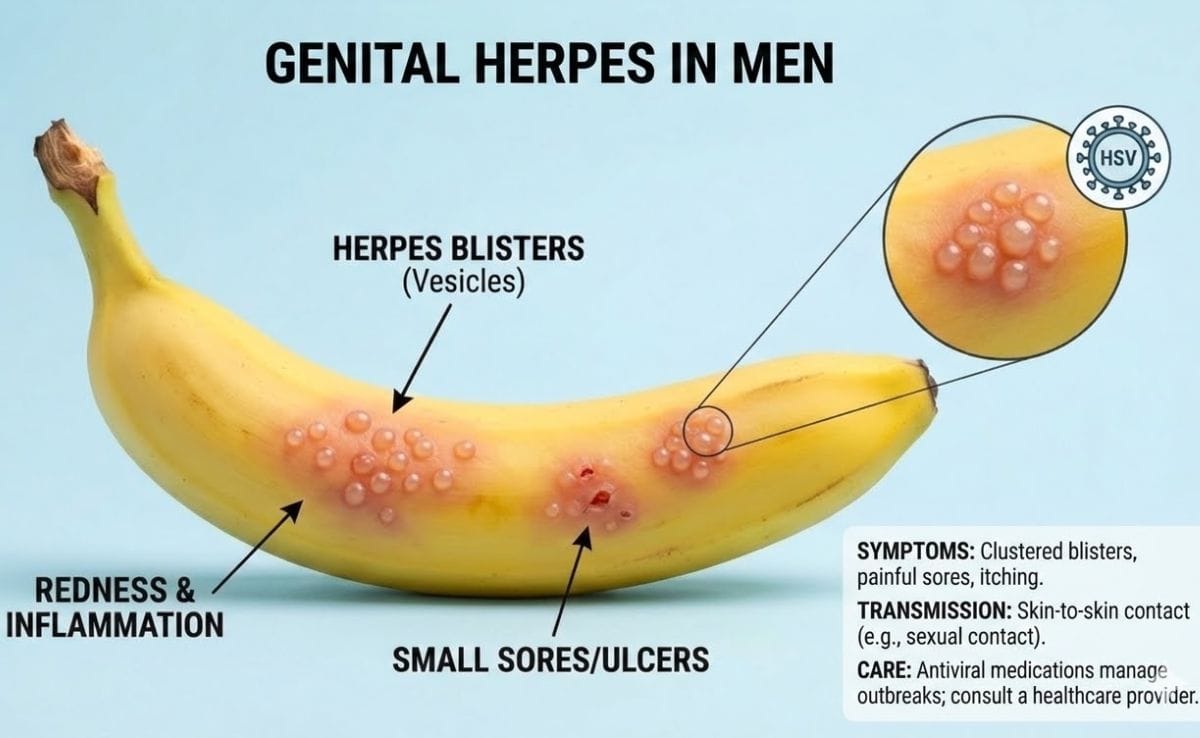
In men, genital herpes often presents in ways that are physically uncomfortable and psychologically disruptive, especially during the first few outbreaks.
Common symptoms men may experience
Sores most commonly appear on the penis or along the shaft, around the foreskin, or near the head. They can also develop on the scrotum, groin, inner thighs, or around the anus. The location depends on where the virus entered the skin.
Before sores appear, many men notice a warning phase: tingling, sensitivity, or a burning sensation in a specific spot. This is often ignored until blisters become visible.
If sores form close to the urethral opening, urination can become painful. Some men describe a sharp stinging sensation rather than constant pain, which leads them to delay seeking help—assuming it will settle on its own.
How it affects urination, sex, and confidence
Physical symptoms are only part of the picture. Pain during urination, especially in children with phimosis, can make something as routine as using the toilet stressful. During outbreaks, sexual activity often becomes uncomfortable or impossible, which can strain relationships and self-image.
Many men struggle more with the emotional side than the physical one. Fear of transmitting the virus, uncertainty about disclosure, and anxiety around future relationships are common concerns especially when information online is alarmist or misleading.
With early diagnosis and proper medical guidance, outbreaks become more predictable and manageable. Just as importantly, understanding how the virus works helps men regain confidence and make informed decisions about sex and intimacy instead of avoiding them altogether.
Genital Herpes in Women

Genital herpes can be more difficult to recognise in women, not because it behaves differently, but because symptoms are often less visible and easier to misinterpret.
Why are symptoms harder to detect in women?
In women, sores don’t always appear externally. They can develop inside the vagina or on the cervix, where they aren’t easily seen without an examination. When sores aren’t visible, symptoms tend to present as discomfort rather than obvious lesions.
Many women experience itching, burning, unusual sensitivity, or pain during urination. Because these symptoms overlap with common conditions like yeast infections or urinary tract infections, herpes is frequently overlooked, especially when symptoms improve temporarily.
Another issue is recurrence. Mild outbreaks may cause only vague irritation, leading women to treat themselves repeatedly with antifungal creams or antibiotics without realising the underlying cause hasn’t been addressed.
Risks during pregnancy and gynaecological health
For most women, genital herpes doesn’t interfere with fertility or everyday gynaecological health. The main concern arises during pregnancy, specifically around delivery.
If a woman has an active outbreak close to labour, there is a risk of transmitting the virus to the baby during vaginal delivery. This is why obstetric care includes careful monitoring and, in some cases, preventive antiviral treatment in the later stages of pregnancy.
With proper medical management, the majority of women with genital herpes deliver safely and without complications. The key is awareness and early communication with healthcare providers, not fear or avoidance.
Does genital herpes go away on its own?

The visible part does; but the virus itself doesn’t. For those looking for long term solutions, we urge men to explore their options to treat genital herpes, especially for those seeking long-term relationships. During an outbreak, blisters and sores eventually heal, often without treatment. This healing phase is what convinces many people that the problem has been resolved. In reality, the herpes simplex virus remains in the body, lying dormant in nearby nerve cells.
When the immune system is under stress, whether through illness, lack of sleep, emotional strain, or hormonal changes, the virus can reactivate. For some people, this happens once every few years. For others, it’s more frequent. The pattern heavily varies depending on the individual.
Long-term health risks you should actually care about
Genital herpes is rarely dangerous in the traditional medical sense. It doesn’t damage organs, shorten lifespan, or affect fertility in healthy adults.
The real risks lie elsewhere. Open sores increase vulnerability to other sexually transmitted infections, particularly HIV, because broken skin makes transmission easier.
There’s also the psychological and social impact. Recurrent outbreaks, fear of passing the virus on, and anxiety around disclosure can weigh heavily if the condition is misunderstood or left unmanaged. Many patients report that uncertainty and stigma affect them more than the physical symptoms themselves.
How Is Genital Herpes Diagnosed?
Diagnosing genital herpes isn’t always straightforward. Many patients having confusion often comes from testing at the wrong time or relying on a single test result without proper clinical context.
Swab tests & blood tests
When active sores are present, a swab test taken directly from the lesion is the most reliable way to diagnose genital herpes. This test looks for viral genetic material and can usually confirm both the presence of herpes and the virus type.
Blood tests work differently. They detect antibodies, which indicate past exposure to the virus; but not necessarily where the infection is located or whether current symptoms are caused by herpes. A positive blood test could reflect an old oral infection rather than an active genital one.
This is why doctors often prioritise swab testing when lesions are visible and use blood tests selectively, rather than as a blanket screening tool.
When testing gives false negatives
Timing plays a critical role in accuracy. If testing is done too early before the body has produced detectable antibodies, blood tests may return negative even though infection has already occurred. On the other hand, once sores have healed, swab tests lose effectiveness because there’s no active virus on the skin to sample.
False reassurance is another common issue. A negative result taken at the wrong time can delay diagnosis and prolong uncertainty. This is why clinical judgement from assessing symptoms, exposure history, and timing matters just as much as the test itself.
In practice, accurate diagnosis often involves follow-up testing or monitoring rather than a one-off result.
How to Reduce the Risk of Spreading Genital Herpes

Avoid sexual contact during outbreaks
This is the single most effective step. When sores or early warning signs like tingling and burning appear, the virus is most active on the skin. Sexual contact during this phase significantly increases the chance of transmission.
Even if sores seem minor or are already healing, it’s best to wait until the skin has fully recovered. This applies to all forms of sexual activity, not just penetrative sex.
Use protection consistently, but there are limits
Condoms and dental dams reduce the risk of transmission by limiting skin contact, but they don’t cover all genital areas. This means protection lowers risk rather than eliminating it completely.
Consistent use matters more than occasional use. Many transmissions happen during moments when protection is skipped because symptoms aren’t visible.
Be aware of asymptomatic viral shedding
Genital herpes can spread even when there are no visible sores. This asymptomatic shedding is unpredictable and varies from person to person.
Understanding this helps set realistic expectations. A lack of symptoms doesn’t equal zero risk, it just means the risk is lower than during an active outbreak.
Consider daily suppressive antiviral therapy
For people with frequent outbreaks or those in long-term relationships, daily antiviral medication can significantly reduce both recurrence and transmission risk.
Suppressive therapy doesn’t replace safe practices, but it adds another layer of protection especially when combined with consistent communication and protection use.
Communicate openly with sexual partners
Open conversations allow partners to make informed decisions together. While disclosure can feel uncomfortable, it builds trust and reduces anxiety over time.
常见问题解答
There’s no instant fix, but starting antiviral medication early, ideally at the first sign of tingling or discomfort can significantly shorten an outbreak. Keeping the affected area clean and dry, avoiding friction, and getting enough rest also help the body heal more efficiently.
No. Home remedies may ease discomfort, but they don’t eliminate the virus. Genital herpes is caused by a virus that remains in the body, and proper medical treatment is required to manage it effectively. Relying solely on home treatments often delays diagnosis and allows outbreaks to recur unnecessarily.
Living normally with genital herpes comes down to understanding the condition and managing it proactively. Many people have long symptom-free periods and maintain healthy relationships, careers, and sex lives.
Once outbreaks become predictable or controlled, herpes tends to fade into the background rather than dominate daily life.
Physically, genital herpes rarely causes serious long-term health problems in healthy adults. The more significant effects are often psychological such as stress, anxiety, or fear of transmission, especially when the condition is poorly understood.
With proper information and care, these concerns are manageable and often lessen over time.
Yes. Genital herpes doesn’t define your health, your relationships, or your future. With treatment, awareness, and open communication, most people live full, normal lives without frequent symptoms or complications.
Take Control of Your Sexual Health Today at He Medical Clinic
Genital herpes is manageable but only if it’s properly diagnosed and treated. If you’re experiencing symptoms or need confidential advice, book a consultation at He Medical Clinic today and get clear answers, not guesswork.
Your health, comfort, and privacy come first.